Leadership and Improvement During Disruption: Scaling Vaccinations
We are seeing an air of hope as healthcare continues to play a critical public role toward managing the impacts and ongoing challenges of the COVID-19 pandemic. The latest phase, and perhaps the most critical, is to provide vaccinations at increasing levels each day all while supplies are uncertain and varying, staff and volunteers are stretched thin, and there’s a need to remain nimble as things change daily and weekly.
In this phase, dynamic healthcare leaders are taking this moment to reflect on how COVID-19 has become a learning springboard to unlock their thinking to become something better. By moving from a short-lived “process flows and improvement mindset,” to one anchored in understanding improvement science and flow methodology, these leaders will provide a means to sustainability and successful adaptive change.
Two Crucial Concepts for Healthcare Leaders
As leaders chart their journey forward, two key concepts are integral to understand.
1. VMPS Flows of Medicine™
The VMPS Flows of Medicine™ is a comprehensive and foundational framework for creating superior patient flows. Understanding and managing the various flows can drive swift and effective change bringing order where disruption may otherwise take hold. Using this framework can serve as a foundation for your process study and analysis so you can clearly grasp your current state before leading improvements for your future state.
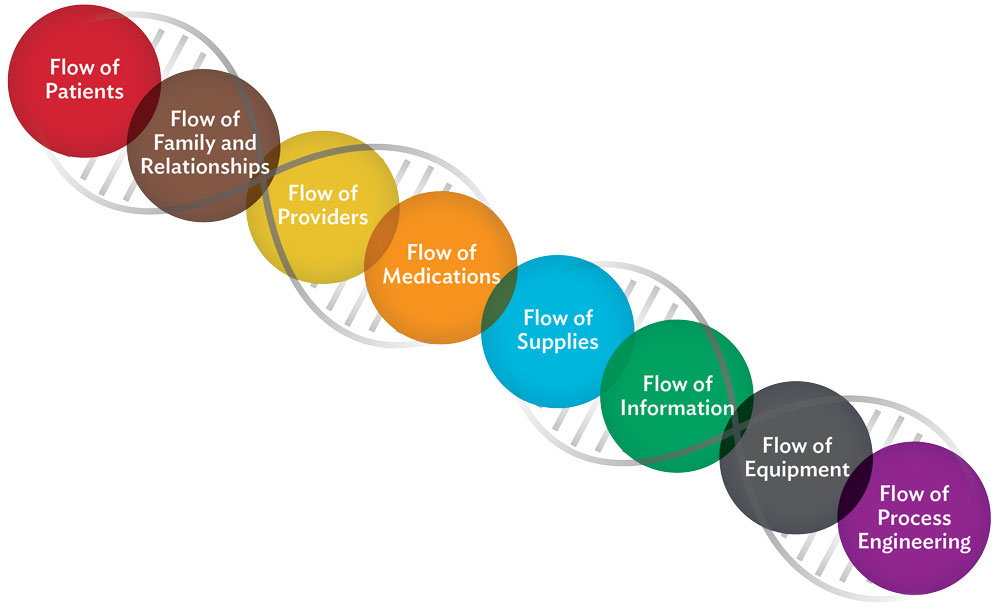
2. Leadership’s Role in Driving Change
Leaders who can clearly articulate a broad vision and provide inspiration, frame the known issues, establish accountable teams, and support them by removing barriers will be best positioned to achieve the desired outcomes and establish a foundation for ongoing sustainability and scale
Recent examples from our partners’ vaccine distribution efforts provide lessons in how applying the Flows of Medicine with effective leadership can help you continue to manage and improve your processes and stay nimble as you manage through this next wave of your COVID response.
Case 1 | 33% Increase in Vaccine Throughput with Existing Resources
Client: University Medical System – Western U.S.
The challenge: Provide more vaccinations while reducing waiting time.
The application: Working with Sensei Chris Backous, the team studied the current state flows of patients, supplies, providers and overall site layout and determined that a few key changes could unlock additional capacity. The client team planned their Plan-Do-Study-Act cycles (PDSAs) to improve flow and reduce wait time and scheduled their first tests of change for the lower-demand evening hours just a few days later.
The outcome: Through real-time simulation and implementation of their changes, the team was able to increase vaccine throughput by 33% and reduce patient wait times using existing resources.
Case 2 | Three Days to Mass Vaccination Site Success
Learning Lab: Virginia Mason Medical Center – Seattle
Note: Virginia Mason Medical Center remains an epicenter for innovation. Many of the breakthrough improvements developed from our Virginia Mason “learning lab” serve as the creativity jump start to help accelerate improvements for our Institute partners.
The challenge: Virginia Mason had short notice to partner with a Seattle tech giant to put on weekly “SuperVax” mass vaccination events where more than 2,000 individuals were to be vaccinated each day using this corporate partner’s downtown Seattle space, volunteers and logistics, Virginia Mason Medical Center’s staff and volunteers from the community.
The application: The Virginia Mason Production System®, the integrated management and improvement system designed by and for healthcare organizations, provided a foundation for planning with executives and the operational leaders tasked with managing this effort. Documenting the Flows of Medicine alongside rapid cycle PDSA simulations allowed teams to complete much of the planning for an initial event in just three days.
The outcome: The goal of vaccinating 2,000 people was surpassed during the first event. The event ran effectively with limited issues served as a platform for follow-up events with continued improvements and expansion.
Lessons learned and further preparation: Each vaccination event is followed by a review of lessons learned and identified opportunities for improvement. Learnings have led to the expansion of the event to span two days as vaccine supply becomes available to vaccinate even more community members each weekend. Review and reflections may also bring up the need for additional improvement events – a recent example being a half-day innovation event to standardize the initial process.
Breaking it Down: Orchestrating the Flows of Mass Vaccination
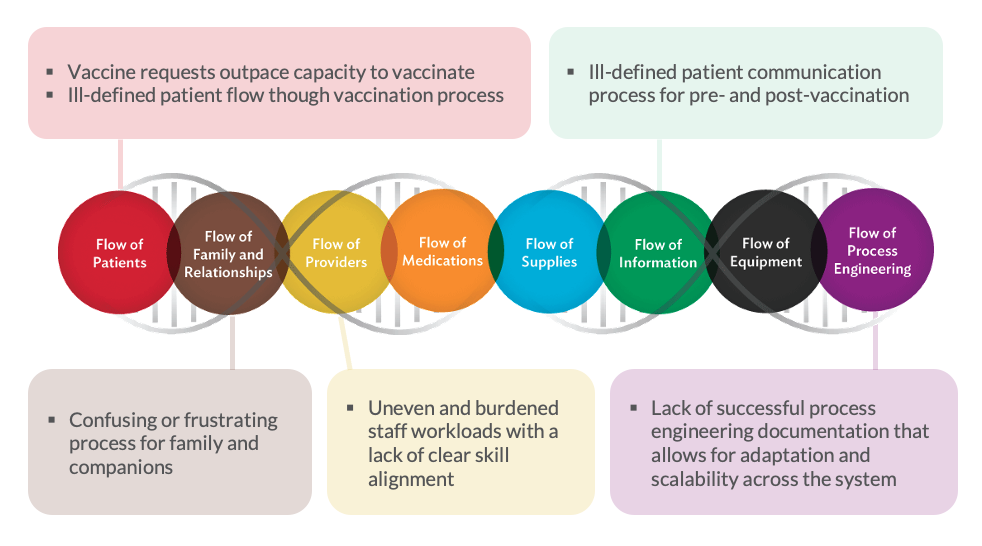
Driving large scale operational change requires systems thinking, acting strategically, and engaging and supporting team members in the necessary work to understand current state and design their future state. Mastering systems thinking begins with the process study and analysis anchored in the Flows of Medicine. Using a unified and proven set of tools, methods and repeatable leadership routines provides the foundational thinking that can jumpstart this body of work and enable sustainable and scalable processes. Examples of common COVID vaccine challenges that drove subsequent improvements are linked to the Flows of Medicine breakdown below.
We’re proud of the progress of many of our clients including this honor described by Prof Andy Hardy, CEO, University Hospital Coventry and Warwick NHS Trust, sharing his thoughts on some of the reasons why they were selected as the first COVID Vaccination site in the world.
“The partnership we have shared with Virginia Mason over the last five years has completely transformed UHCW. The cultural aspects of embedding lean thinking into our hospitals has spring boarded us towards our vision ‘to be a national and international leader in healthcare’; this was most recently evidenced by us being the site of the first COVID vaccination in the world. One of the reasons that we were chosen was the embedding of our improvement system UHCWi, which was developed in conjunction with VMI, and enabled the organisation to “learn fast” during the first wave of COVID, facilitated by such tools as PDSA being embedded in every part of the organisation. We constantly work under the banner of putting the patient first and understanding that, better never stops.”
The foundational principles of the Virginia Mason Production System® can help you as you work to bring vaccinations to your team members and community. They can be applied to the administration of 50 vaccines a day or 5000. To learn more about how we and client organizations have applied the principles of the Virginia Mason Production System® to our response to COVID-19, visit our Resource page and search COVID to find blogs, case studies and webinars.
If you want to talk through your specific challenge you are facing with your vaccination program, click here to request a complimentary 30-minute consult with one of our Transformation Advisors.
Executives and Senior Leaders
Develop your ability to purposefully contribute to bringing order, removing barriers, and empowering your teams.
Download our eight key behaviors for executives and senior leaders
Process Improvement and Operational Leaders
Learn about the three improvement fundamentals you should know for optimizing your vaccine distribution flows.






